
Shared Responsibility: How hospitals can help improve medical device data security
For some time, this notion of a shared responsibility for data security has been recognized as a best practice within the larger technology industry.
Latest release of Philips Capsule Surveillance receives FDA clearance

Live, streaming patient data is available via virtually any browser-based device, to see multiple patients – with deep dive capability to see waveforms, trends, events, history, device settings, and more. The Capsule Surveillance workstation view provides an alert list across multiple patients ordered by priority.
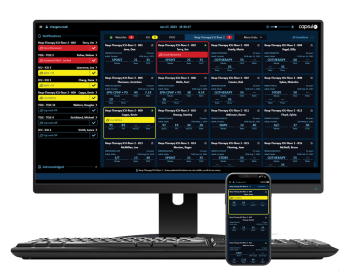
Continuous clinical surveillance can help extend the reach of frontline clinical staff over the full range of intensive care patients, regardless of where they receive care in the facility. Ventilated Patient Surveillance provides a centralized view of ventilator data and annunciates clinically actionable emergent events:
The need for solutions that alert clinicians to emergent, clinically actionable events is increasing due to the rising acuity level of patients throughout the hospital, and the continuing shortage of nurses, respiratory therapists and other care providers.
Clinical surveillance involves the analysis of live-streaming clinical data from all patient devices using condition-specific algorithms.
As part of implementation, Capsule specialists can work with clinical staff to configure Smart Rules for the facility and specific care areas. Capsule Surveillance allows for rules customization aligned with clinician preferences and practices. Certain Capsule Smart Rules support established, published clinical practice guidelines.
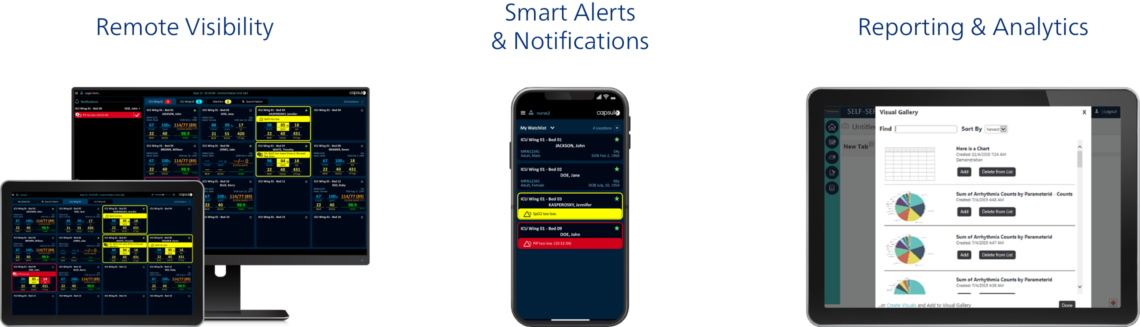
Through Smart Rules, Capsule Surveillance performs a multi-variable assessment of a patient and notifies caregivers with Smart Alerts when the patient’s condition shows signs of deterioration that can potentially lead to emergent events. Through Smart Alert distribution to the assigned care team members’ mobile devices or other remote screens, these notifications are made available to caregivers on the go or those who provide additional oversight, such as in an eICU or virtual care setting.
Capsule Surveillance brochure
DownloadCapsule Ventilated Patient Surveillance product brief
Download
For some time, this notion of a shared responsibility for data security has been recognized as a best practice within the larger technology industry.

High-quality data gives medical researchers and clinicians the level of detail they need to better be able to study the efficacy of treatments and identify patterns and trends in healthcare outcomes.